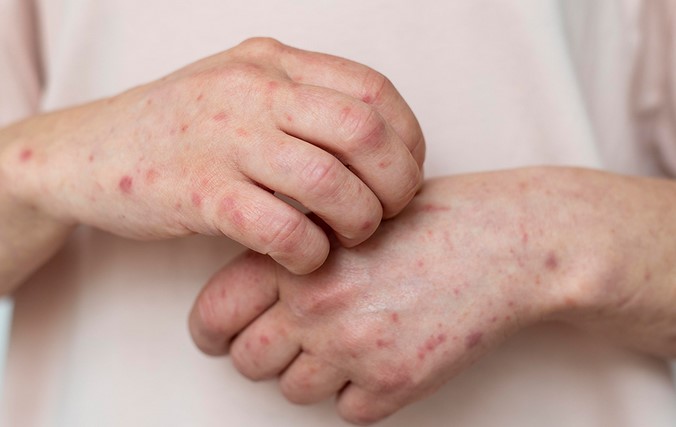
You’re lying in bed at 3:00 AM, and the itch isn’t just a tickle—it’s a demanding, burning roar that feels like it’s coming from deep beneath your skin. You know that if you scratch, you’ll break the surface and bleed, but the sensation is so overwhelming that logic flies out the window. Statistics show that over 31 million Americans live with some form of eczema, meaning millions of people are likely staring at the ceiling right now, just like you, wondering why their skin has turned against them.
In my decade of writing for the health industry and working closely with dermatological experts, I’ve seen that the biggest hurdle in managing eczema flare-ups isn’t a lack of creams—it’s a lack of strategy. I’ve sat in rooms with patients who have tried every “miracle oil” on the internet, only to realize they were inadvertently stripping their skin’s defenses every morning in the shower. True relief comes when you stop “attacking” the itch and start “rebuilding” the fortress.
The Cracked Brick Wall: Understanding the Skin Barrier
To understand eczema (or atopic dermatitis), think of your skin as a brick wall. In healthy skin, the cells are the bricks, and lipids (oils) are the mortar. This wall keeps moisture in and keeps “intruders” like allergens, bacteria, and irritants out.
In a person with eczema, the mortar is thin or missing. The wall becomes porous, moisture leaks out (a process called Transepidermal Water Loss or TEWL), and irritants crawl through the gaps. When these intruders get inside, your immune system panics and sends in an “army” of inflammation, which results in the red, itchy, and scaly patches we call a flare-up.
Immediate Steps for Managing Eczema Flare-Ups
When you are in the middle of a crisis, the goal is to calm the immune response and manually seal the gaps in your “wall.” Here is the tactical approach I’ve seen work most effectively for those in the beginner and intermediate stages of their journey.
1. The “Soak and Seal” Method
This is a cornerstone of clinical treatment. You take a lukewarm (never hot!) bath or shower for 10 minutes. Immediately after stepping out—within three minutes—pat your skin slightly dry and apply a thick layer of emollient. This traps the water in the skin before it can evaporate and pull more moisture out with it.
2. Identifying and Neutralizing Triggers
You cannot manage a flare if you are still pouring gasoline on the fire. Common triggers include:
-
Scented Products: “Fragrance” is a vague term for hundreds of chemicals that trigger the immune system.
-
Temperature Swings: Moving from a cold, dry outdoors to a blast of indoor heating is a classic recipe for a winter flare.
-
Stress: High levels of cortisol can weaken the skin barrier further, creating a cycle of “itch-stress-itch.”
Advanced and Technical Treatment Options
As you move into the intermediate phase of managing eczema flare-ups, you might need more than just over-the-counter (OTC) lotions. This is where medical intervention and specific technical treatments come into play.
Topical Corticosteroids and Non-Steroidal Creams
For years, topical corticosteroids have been the first line of defense to shut down inflammation. However, intermediate users should also be aware of calcineurin inhibitors (like tacrolimus) or PDE4 inhibitors. These are non-steroidal options that help control the immune response without the risk of skin thinning associated with long-term steroid use.
Wet Wrap Therapy
For severe, stubborn flares, we often recommend wet wraps. After the “soak and seal” process, you apply a layer of medication or moisturizer, wrap the area in a layer of damp gauze or cotton clothing, and then add a dry layer on top. This dramatically increases the absorption of the treatment and provides a physical barrier against scratching.
Understanding the Microbiome
Recent research has highlighted the role of Staphylococcus aureus—a bacteria that often overcolonizes eczema skin. In my experience, if a flare-up looks “weepy” or has golden crusts, it may be infected. Treatments like diluted bleach baths (supervised by a professional) act like a “reset button” for the skin’s bacterial balance.
Technical Context: LSI Keywords for the Savvy Patient
To navigate your dermatology appointments effectively, you should be familiar with these terms:
-
Filaggrin: A protein that helps keep the skin barrier strong; many eczema sufferers have a genetic mutation that produces less of it.
-
Pruritus: The medical term for itching.
-
Lichenification: Skin that has become thick and leathery due to chronic scratching.
-
Immunomodulators: Medications that change the way the immune system reacts to triggers.
-
Hypoallergenic vs. Non-Comedogenic: While “hypoallergenic” means less likely to cause an allergic reaction, it is not a regulated term. Look for “fragrance-free” and “dye-free” instead.
Pro-Tips and Hidden Warnings
The “Hidden Warning”: Beware of “Natural” DIY recipes involving food products like lemon juice, undiluted apple cider vinegar, or certain essential oils. While they sound healthy, the high acidity or volatile organic compounds can actually cause a chemical burn on a compromised eczema barrier. Always patch test on a small area of healthy skin first.
Tips Pro: Switch to a silk or bamboo pillowcase and bedsheets. Traditional cotton can actually be quite abrasive under a microscope, and it absorbs the expensive creams right off your skin while you sleep. Synthetic or silk fabrics glide over the skin, reducing the mechanical irritation that triggers the “itch-scratch cycle” at night.
The Long Game: Maintenance and Prevention
Managing eczema flare-ups is 20% about the flare and 80% about what you do when your skin looks “fine.” Maintenance is boring, but it’s the only way to prevent the next 3:00 AM wake-up call.
-
Ceramide-Rich Moisturizers: Look for products that specifically mention ceramides on the label. These are the “mortar” molecules your skin is missing.
-
Dietary Awareness: While not everyone has a food trigger, some find that highly processed sugars or dairy can increase systemic inflammation. I suggest keeping a “Skin Diary” for two weeks to see if your flares correlate with specific meals.
-
Laundry Habits: Use an extra rinse cycle for your clothes and towels to ensure every trace of detergent—even the “free and clear” ones—is gone.
Summary: Empowerment Over the Itch
Eczema can feel like a life sentence of discomfort, but it is a manageable condition. By understanding that your skin is simply a “leaky wall” that needs constant reinforcement, you take the power back from the itch.
In my ten years of observing these patterns, the people who find the most success are those who remain consistent. Don’t wait for the red patches to appear to start your “Soak and Seal.” Treat your skin with the gentleness it deserves every single day.
What is the one trigger you’ve identified that always seems to set your skin off? Identifying your “enemy” is the first step toward a flare-free life. Share your experience in the comments below—let’s help each other build better barriers!